Younten Tshedup
Over the last five years, multidrug-resistant (MDR) tuberculosis (TB) cases have been steadily increasing in the country, which is a major public health concern today.
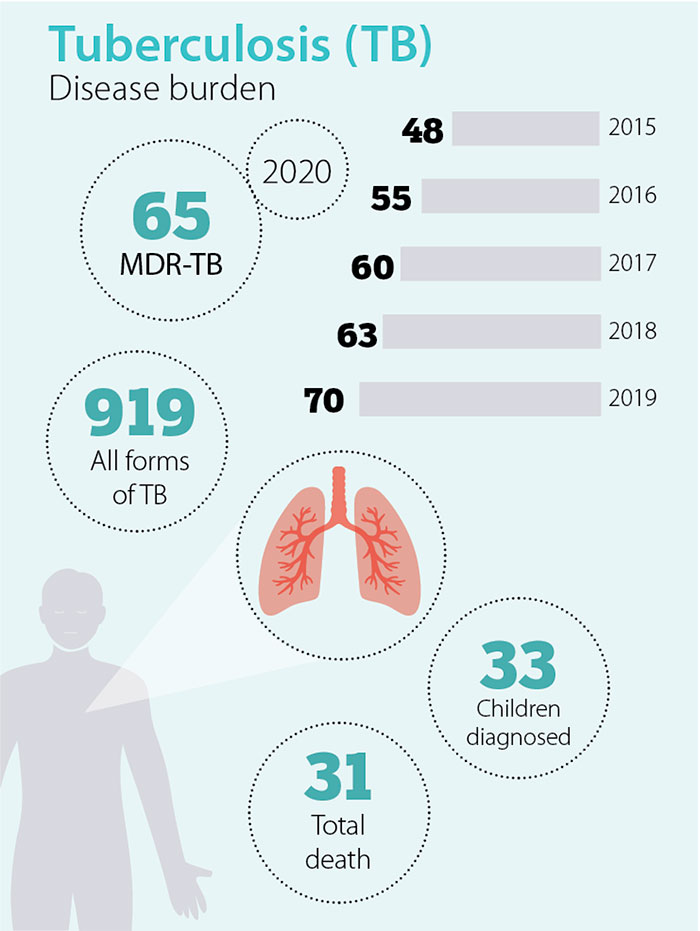
MDR-TB has annually increased by about 15 cases on an average. There were 65 cases last year.
Records with the health ministry show that the country had 919 cases of TB (all forms), including MDR TB last year.
The disease has killed 31 people so far.
Chief of communicable disease division, Rixin Jamtsho, said that TB was still a priority public health problem in the country today that mostly affected the productive age groups of 15-44 years (73 percent).
“It’s one of the oldest diseases but still remains one of the world’s deadliest and infectious killers,” he said. “Globally, TB claims nearly 4,000 lives everyday; close to 28,000 people fall ill with this preventable and curable disease.”
Rixin Jamtsho said that, in Bhutan, besides reducing the productivity of those infected, the disease also added significant burden on the economy, as people needed extensive treatments.
Like other communicable diseases, TB can spread from one person to another very easily when a sick person with TB expels bacteria into the air by coughing or sneezing.
He said that, despite the progress made in rate of TB case detection and achieving high treatment success in the 2019 cohort, the number of MDR-TB cases has been increasing in the country.
Bhutan today has one of the highest incidences of MDR-TB cases in the South Asia region.
MDR-TB is caused by TB bacteria (Mycobacterium tuberculosis), which is resistant to at least two medications — isoniazid and rifampin — the two most potent TB drugs. These drugs are used to treat all persons with TB.
While the country recorded 919 cases of TB last year, a slight decrease from 2019 (1,016 cases), the World Health Organisation (WHO) 2020 Global TB Report, states that an estimated 1,300 all forms of TB cases are seen in Bhutan.
This means that there is a detection gap where people with TB go undetected. The current detection gap stands at around 30 percent for drug-sensitive TB (DSTB) and 66 percent for MDR-TB.
Rixin Jamtsho said that slow contact tracing and inadequate diagnostic facilities added to the detection gap in the country. He said that, besides the detection gap, MDR-TB cases among new TB patients and patients not taking medicines regularly were some of the other challenges in managing TB in Bhutan.
However, he added that, despite the challenges posed by the Covid-19 pandemic, the health ministry and the national TB control programme did not face any disruption in providing TB services and interventions to the general public.
Also, the flu clinics set up in the wake of the pandemic helped the programme detect 58 TB and seven MDR-TB cases last year.
Several interventions have been put in place to combat the disease in the country, which includes implementation of aggressive contact tracing among close contacts of TB and MDR-TB cases, TB screening and testing for targeted and risk groups, expanding GeneXpert sites in high burden dzongkhags, and ensuring uninterrupted supply of TB medicines, among others.
The ministry has also set an ambitious target to make TB no longer a public health problem by 2030. It plans to increase case notification rate of at least 90 percent among estimated TB and MDR-TB cases, and ensure 90 percent treatment success rate for DSTB and 75 percent for MDR-TB.
The World TB Day (March 24) this year was observed with the theme “The clock is ticking” to indicate that the world was running out of time to act on the commitments to end the deadly disease.
TB is one of the top 10 causes of death among the communicable disease globally.

